

Bilateral endoprosthesis replacement of the hip and knee joint
Joachim Pfahl, Philip Höhle, Philip Rebain
RESUME
Background: In Germany, more than 300,000 operations for hip endoprosthesis replacement are performed every year. Given the ever-increasing number of operations, simultaneous replacement of the hip and knee joints is considered. This replacement is considered for bilateral symptomatic arthrosis.
Methods: This publication is based on the selective literature study and the results of own prospective comparative studies of simultaneous replacement of the hip joint.
Result: During the simultaneous replacement of the hip, the difference between the number of lethal cases and the incidence of diseases will not be considered as compared to the one-site operation. Rehabilitation is easier after bilateral surgery. A slightly increased mortality rate (0.30% to 0.14%) in relation to the incidence after surgery on the knee joint is not a difference compared to the one-way operation.
In the bilateral operation, especially on the knee joint, there is a great need for blood transfusion.
As with the replacement of the hip joint, and when replacing the knee joint, it is more expedient to perform bilateral surgical intervention than the two-step operation to replace joints in the inpatient department.
Conclusion: When replacing the hip joint, the most reliable method for patients, regardless of age and the ASA scale (AAA, American Association of Anesthesiologists), is the two-way replacement. It is also characterized by a favorable rehabilitation process.
Since there is a high risk of having the blood transfusion or lethal outcome when replacing the knee joint, the authors recommend the two-sided replacement of joints for patients with 1 and 2 category according to ASA. Costs for bilateral replacement of joints are half that of two separate operations.
References:
Pfahl J., Höhle P., Rebain P. Two-sided endoprosthesis replacement of the hip or knee. German International Medical Bulletin, 2011;
108(■■): ■■-■■. DOI: 10.3238/arztebl.2011.0nn
In Germany in 2008 The Federal Service for Quality Control recorded the implantation of about 158,000 hip joints and 147 000 implants of knee joints. This shows the quantitative value of the endoprosthesis replacement of these joints. Bilateral simultaneous endoprosthesis replacement is not included in this statistic, since it displays a different group of cases (DRG, diagnostics of related groups). Some patients have indications for bilateral prosthetics. A decisive criterion in favor of simultaneous bilateral replacement is bilateral severe symptomatic osteoarthritis and the patient’s desire to replace both joints. By improving operational planning, easier insertion of implants and sparing muscular surgical techniques, it is obvious that there is a choice of bilateral replacement of joints.
The purpose of this review is to consider the pros and cons of simultaneous and bilateral endoprosthesis replacement for the patient. Randomized controlled trials comparing bilateral joint endoprosthesis replacement with the two-step operation do not exist. For this reason, the evidence of the presented results is limited.
Methodology
This review article is based on the selective literature study and the results of own prospective comparative studies of simultaneous replacement of the hip joint. Below, there are the data from the Orthopedic Clinic of St. Joseph Hospital, in Wiesbaden, the prospective comparative study of the simultaneous replacement of the hip joint (30 bilateral and 30 unilateral operated patients) with evaluation.
There are no selected Cochran approaches or guidelines for choosing a procedure to replace bilateral joint aging.
History
The history of endoprosthesis replacement of large joints began in the middle of the 20th century. As early as 1971, publications appeared that addressed the question of whether to give preference to bilateral total hip endoprosthesis replacement with bilateral coxarthrosis.
The aim of this study of 50 bilateral patients was to find out whether the new treatment method is as successful as one-sided endoprosthesis replacement, goes hand in hand or even has an advantage in patients. The main subject of this study was the evaluation of functional or clinical results. The results were promising. There were many publications devoted to the topic of simultaneous replacement of joints on both the hip and the knee.
The results obtained in recent years have provided answers to the questions arising here based on some prospective comparative studies.
Frequency of bilateral joint replacement
Whether simultaneous endoprosthesis replacement is offered to the patient, it will largely depend on the surgeon. Clinics with many procedures often offer this option. The highest rates of unilateral endoprosthesis replacement of the hip as a percentage of the Clinic in Vrigtington in England. Over a 20-year period, 13,000 operations were performed there, of which 405 were bilateral. This corresponds to 3.1% of patients and, respectively, 6.2% of used prostheses.
In the last three years (2008-2010) at St. Joseph Hospital in Wiesbaden, hip endoprostheses were implanted in 1692 patients, and 62 simultaneous replacements were performed. It corresponds 3.7% of all patients with operated hip joints. In North America and Asia, the largest number of patients had replacement of the knee joints. In one retrospective Korean study report, Kim reports about more than 2,385 simultaneous endoprosthesis replacement of the knee joints. How often simultaneous bilateral operations were carried out all over the world is unknown.
There are regional differences. In South America, this approach, unlike in North America and Asia, is little used. On the simultaneous replacement of hip or knee joints, there are numerous publications. In contrast, this procedure for ipsilateral osteoarthritis of the hip and knee joints or arthrosis of all four joints is little considered.
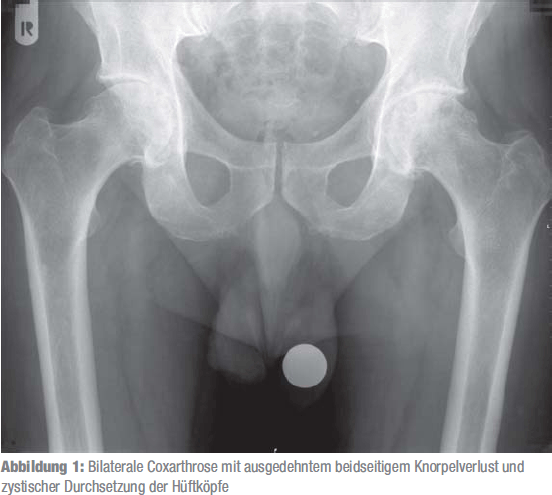
Figure 1 demonstrates the expressed bilateral hip arthrosis of the patient who decided to replace simultaneously both joints. Figure 2 shows the digital pre-operational planning on the scaled image, which presents the virtual placement of joint prostheses. Figure 3 shows the situation after simultaneous endoprosthesis replacement of the hip joint.
Safety of simultaneous endoprosthesis replacement
Selective endoprosthesis replacement of the joint is associated with a low mortality rate. In various composite studies, numbers from 0.14 to 0.3% are indicated. All published data – retrospective or prospective studies in the context – with respect to simultaneous replacement of the hip joint show no difference. There was also no large retrospective study of the difference in mortality between low-risk patients (ASA classification 1-2, ASA, American Society of Anesthesiologists) and high-risk (ASA classification 3-4). The ASA classification of operated patients in Germany (2008) was published by the Federal Service for Quality Control (BQS) and is shown in Table 1 below. A retrospective study of 450 unilaterally operated patients compared with 450 bilateral operated patients who underwent surgery from 1970 to 1997 showed the higher level of pulmonary embolism (1.6% compared to 0.7%). Mortality during the first year after surgery is again higher in unilaterally operated patients (4% vs. 3.1%). All patients received prior to 1986 warfarin for prevention.
Since 1987, prophylaxis only on the day of surgery was performed with heparin and only 325 mg of aspirin a day is prescribed for prevention from the first postoperative day. So far, these data are not comparable with the prevention for four weeks, which is practiced in Germany, where used with low-molecular-weight heparin or new oral antithrombotic drugs.
Concerning the knee joint, there are various details concerning the threat to the life of the patient when replacing the joint. Again, in many studies there is no difference. In the analysis of all prosthetic knee joints delivered in the United States between 1998 and 2006, the mortality rate after bilateral surgery was 14%, 0.30% after unilateral operations (p <0.0001). If the second side is operated during the hospital stay, the incidence rate and the risk of mortality increase. In the prospective study, 70 patients who were older than 70 years who underwent endoprosthesis replacements were compared with the control group of 312 young patients with unilateral total endoprosthesis replacement of the knee. The risk of diseases is comparable; the risk of mortality was not considered. The authors do not see the senior age as a contraindication for simultaneous bilateral endoprosthesis replacement. In addition, for simultaneous bilateral endoprosthesis replacement of the hip joint a comparative study of patients who were 75 years of age or older (n = 43) and younger patients was published (n = 136) (retrospectively). In this study, too, there was no difference.
Frequency of complications
In the joint endoprosthesis replacement, there are various possible complications, however, which are rare. It is necessary to distinguish in general thromboembolic events and specific complications associated with the corresponding surgical procedure. Two potential comparative studies between simultaneous replacement and unilateral replacement of the hip joint did not show differences in the ratio of fat embolism and respiratory depression in procedures. It is interesting that patients with bone embolism of the brain are significantly less saturated with oxygen on the first postoperative day than patients without embolism (p = 0.017). However, this was in both groups. Several studies that showed thromboembolic complications during simultaneous replacement of hip joints could not detect any differences. In the meta-analysis, which was based on 23 separate studies and 2,063 bilateral endoprosthesis replacements of the hip joints, no statistically significant difference was found (p = 0.365 and p = 0.268). In their own study, a total of 60 patients and no thromboembolic complications were observed.
Even with specific complications (infections, fractures and dislocations), differences in many studies are not visible. The largest studies of simultaneous replacement of knee joints retrospectively analyzed 2385 simultaneously bilateral and 719 unilateral prosthetic patients showed no differences. Berend and others saw 1.4% (bilateral) versus 1.3% of cases of deep infection associated with implanted hip joints. The rate of infection is still low today. Thus, the authors of this study observed over more than one thousand implanted hip joints in the last two years, and only 0.4% of cases had deep infections.

Loss of blood and transfusion
The frequency of blood loss during bilateral endoprosthesis replacement is logically higher than that of a unilateral one. In own studies, the hemoglobin level was 14.1 mg/dl on the first day after the operation, on average 10.2 mg/dl, compared with 11.0 mg/dl after the one-sided operation.
Four of the patients operated simultaneously and two unilaterally during the hospitalization were transfused (Table 2). An increase in the transfusion rate can also be seen in other prospective studies. The speed of transfusion with bilateral endoprosthesis replacement of the knee is higher than with bilateral endoprosthesis replacement of the hip joint. Thus, Peak et al. reported that 20% of patients after hip transplantation and 34% of patients after a knee transplant receive blood transfusions. With transfusion, the incidence rate increases significantly when on-site treatment is delayed with surgery.
Assessment of the patient
The possibility of simultaneous joint replacement for many patients is unknown. After extensive consultations, most patients prefer this procedure. Video recordings of patients who are already walking on crutches a few days after the operation are useful when conducting consultations. 29 of the 30 patients who underwent surgery in their own study retrospectively decided again to conduct this procedure. Often patients are very happy that they have chosen bilateral prosthetics.
Rehabilitation
With bilateral arthrosis, after the first unilateral operation there is still a painful sensation of the joint and further interfere with the rehabilitation of the contracture of the unoperated side. Vykman and Olsson found that in connection with this fact, with bilateral coxarthrosis, optimal joint results may not be achieved before joint replacement. Brand et al. added that simultaneous bilateral total endoprosthesis replacement of the hip provides the best conditions for clinical success, because both sides during the rehabilitation will be unloaded. The undesirable sparing of the operated hip joint is thus prevented. Even when the first operated hip joint shows an excellent functional result, the final satisfactory result can only be after the operation of the contralateral aching hip joint. The procedure for simultaneous prosthetics is desirable in terms of optimal recovery and patient satisfaction. Consecutive unilateral endoprosthesis replacement is the significant temporary, psychological and physical burden on the patient. Thus, the total load of two operations, anesthesia, associated risks, two hospitalizations and two subsequent recovery periods should be taken into account. In addition, the long-term result is an advantage for simultaneous replacement with bilateral arthrosis. With the simultaneous replacement of the hip joints, flexion was significantly better compared to flexing joints after the one-sided or step-by-step operations. This was also noted with respect to indicators that characterize the quantitative activity in daily life. There was no difference with respect to the ability to withdraw limbs and pain data.

Economic aspects
In addition, the time of hospitalization and rehabilitation time is much shorter with simultaneous bilateral treatment compared to two unilateral operations.
This is observed in all studies, and the authors see a clear advantage in the cost of simultaneous operations. Thus, in their own study, simultaneously bilateral operated patients on average 15 days on inpatient treatment, while unilateral operated patients on average 12 days; this means that in two separate operations the patient spends 24 days in the hospital. The following statements are examples of economic differences.
Based on the average values of the state of the baseline value (AVSBV), the catalog of the unified system for the pricing of medical services (USPMS) 2009 Hessen, and expense account was compiled for simultaneous bilateral rehabilitation. The results are shown in Table 3. The benefits to payers are significant.
For the hospital, incomes are higher with simultaneous transplantation, but less than the sum of two unilateral operations. The cost of hospitalization and recovery is paid only once with a simultaneous approach and only slightly higher than with the single-step surgical interventions.
Discussion and recommendations
In almost all studies, bilateral replacement is compared with one-sided replacement. Symptomatic bilateral osteoarthritis means the need for a unilateral operation of only one joint. It is logical that the operation for bilateral replacement of joints – with respect to risks – with the risks of two single-site operations should be compared, since the patient must withstand two of these interventions. Therefore, it is considered that simultaneous replacement in many aspects is a particularly safe method of hip joint prosthetics. From this point of view, bilateral prosthetics of the hip joints are preferable. Simultaneous joint replacement is preferable to the two-step operations, in which a similar operation is performed a few days later on another joint.
In every respect – but in particular, because of the increased complications and increased frequency of blood transfusions – this two-step is inferior to simultaneous prosthetics and, therefore, is not applied. An increase in the frequency of blood transfusion with simultaneous replacement of the hip joint in the future when considering the frequency of blood transfusion during a bilateral operation to discuss with the patient. With bilateral prosthetics, the frequency of blood transfusion is significantly increased.
Even a slight increase in mortality, which corresponds to a doubled rate of prosthetics of the one-sided knee joint. This should be taken into account when weighing the simultaneous replacement. The patient’s age is not critical for simultaneous two-sided replacement. An important classification is the ASA scale. This is indicated in some studies, with different estimates being made. The authors recommend bilateral prosthetic repair for patients with symptomatic bilateral coxarthrosis and ASA classification 1-3, which means more than 99% of patients (Table 1). For the most part today, uncemented implants are used. Nevertheless, thanks to modern surgical techniques and implant design, prosthetic joints can work at full load. As for the knee replacement in patients with 3 category according to ASA, the doctors are very cautious. The increase in the possibility of transfusion should also be discussed. For a patient, a simultaneous replacement is uniquely useful. It represents hospitalization and rehabilitation, which does not differ significantly in time from the rehabilitation of the unilaterally operated patient. Expenses for the patient and loss of employment in the field of employment are lower. The functional result also speaks of simultaneous bilateral prosthetics.
Conflict of interest
The authors state that there is no conflict of interest within the meaning of the guidelines of the International Committee of Medical Journal Editors.
Table 1
|
|
THJR |
TKJR |
|
ASA 1 Normal healthy patient |
9.6% |
6.0% |
|
ASA 2 Patient with mild-form diseases |
59.8% |
59.4% |
|
ASA 3 Patient with severe general diseases and limited capacity |
30% |
34.2% |
|
ASA 4 Patient with inactivated general diseases, constant life threat |
0.6% |
0.5% |
|
ASA 5 Patient is at the point of death |
0% |
0% |
Table 2
Comparison of bilateral (n = 30) and one-sided (n = 30) prosthetic knee joints – prospective study data of the St. Joseph Hospital
|
|
One-sided |
Two-sided |
|
Sex distribution, F/M |
15/15 |
16/14 |
|
Average age (years) |
64 |
62 |
|
Average weight |
80 |
81 |
|
Average grade according to ASA |
2.0 |
2.1 |
|
Duration of hospitalization |
12 |
15 |
|
Harris grade before operation |
41 |
39 |
|
Harris grade in 6 weeks after operation |
91 |
90 |
|
VAS before operation |
7.6 |
7.6 |
|
VAS in 6 weeks after operation |
1.0 |
1.1 |
|
Hemoglobin value before operation |
14.1 |
14.1 |
|
Hemoglobin value on the 1st day after operation |
11 |
10.2 |
|
Blood transfusion (patients) |
2 |
4 |
|
Average working time (minutes) |
75 |
100 |
|
Complications |
0 |
1 postoperative trochanter |
|
Changes |
0 |
1 re-fixation of trochanter |
|
Infections |
0 |
0 |
|
Thromboembolia |
0 |
0 |
|
Walking ability (days) |
2.4 |
2.7 |
VAS, visual analogue scale: 0 (no pain) up to 10 (severe pain).
All patients with bilateral simultaneous replacement of the hip joint who were operated between 6/2006 and 3/2009 at St. Joseph’s Hospital were included in the study.
Table 3
|
|
Two-sided simultaneous prosthesis replacement (DRG I36Z) |
2*one-sided prosthesis replacement (DRG I47B) |
Difference |
|
LBFW (€) |
2.868.50 |
2 x 2 868.50 |
|
|
Specific gravity х |
3.344 |
2.366 |
- |
|
Incomes (€) |
9.592.26 |
13 573.74 |
3 981.48 |
|
Expenses of USPMS (€) |
-8 765.76 |
-12 406.06 |
3 640.30 |
|
Earnings (€) |
826.50 |
1167.76 |
341.18 |
Share:
